Rocky Mountain Spotted Fever (RMSF) Treatment in Glendale, CA
*WARNING: this condition is potentially life-threatening. If you or someone you know is experiencing these symptoms, don't wait. Call 911 or go to the nearest emergency room right away. *
Have you recently traveled to the southeast United States, Canada, or Central America and spent time outside? Are you showing flulike symptoms like fever, chills, nausea, and severe headache accompanied by a bright red spotty skin rash? It may be Rocky Mountain Spotted Fever (RMSF), a potentially life-threatening illnesses caused by a tick bite.
If you have RMSF symptoms, seek out medical attention right away. This illness is considered the most serious tickborne ailment, and it can cause complications like kidney failure or brain inflammation.
To speak with a Rocky Mountain Spotted Fever specialist today in Glendale, call (424) 365-1800 or contact Vitality Integrative Medicine online.
What are the symptoms of Rocky Mountain Spotted Fever?
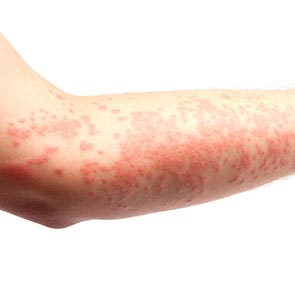
Early Rocky Mountain Spotted Fever symptoms closely resemble those of foodborne illness, flu, or a serious viral infection. The most telling symptom is a Rocky Mountain Spotted Fever rash of small red spots on your wrists, palms, ankles, and soles of your feet that appears two to five days after your fever begins and eventually spreads to your abdomen.
Other symptoms include:
- fever of 102-104
- abdominal pain
- muscle aches and pains
- nausea and vomiting
- fatigue
- poor appetite
- chills
- severe headache
About 10-15% of patients develop no rash at all, and only half of patients report knowledge of a tick bite. For those with rashes, a second rash can develop that's purple-red after five to six days, a strong sign that the condition is worsening.
What causes Rocky Mountain Spotted Fever?
RMSF is transmitted when you're bitten by a tick infected with Rickettsia rickettsii bacteria. These include the American dog tick, the Rocky Mountain wood tick, and the brown dog tick.
When you visit forests, jungles, fields, and other wooded or remote rural areas, you brush against plants and disturb the ticks found on them. This makes the tick leap in search of food.
When a Rocky Mountain Spotted Fever tick bites you, it may draw blood for several days. The longer it's attached to your skin, the greater your odds of getting RMSF becomes. If you attempt to remove the tick carelessly, you can crush it and cause fluid from its body to enter your bite wound and infect you too.
If you take your dog along to outdoor activities like hunting, fishing, or camping, ticks may also seek them out as potential blood sources. The ticks can then jump from your dog onto people.
RMSF is most common in these areas of the world, especially during the times between April to September (tick season):
- Western Canada
- Mexico
- Central and South America
- southern U.S. states like North Carolina, Missouri, Arizona, and Texas
- southern Colorado
- southern and eastern California
Is Rocky Mountain Spotted Fever fatal?
In most cases RMSF is not fatal. However, it can cause severe health complications if left untreated like:
- meningitis (brain inflammation that can cause seizures and coma)
- heart and lung inflammation
- kidney failure
- gangrene (tissue death) in your fingers and toes
- liver and spleen enlargement
- death (rarely)
Leaving RMSF untreated can result in catastrophic consequences, including:
- neurological problems
- hearing loss or deafness
- muscle weakness
- partial paralysis on one side of your body
Some patients, especially the very old, the very young, and people with compromised immune systems (such as HIV/AIDS patients), are at a greater risk of dying from RMSF. Patients with chronic illnesses like diabetes or hepatitis are also at an increased risk of developing severe symptoms like pneumonia, heart failure, and liver failure. However, documented evidence shows that previously healthy patients as young as 18 have contracted fatal cases of RSMF in recent years.1
How is Rocky Mountain Spotted Fever diagnosed?
To diagnose RMSF, your medical provider will ask whether you, a family member, or a co-worker has recently traveled to an area known for RSMF. You'll also be asked whether you spent time in forests, fields, swamps, or other outdoor areas. If not, then it's unlikely that you're suffering from RMSF.
If yes, then an RMSF infection may be possible. To confirm or rule out the disease, your medical provider will inspect your body for attached ticks, a bite area, and the telltale rash. Even if a tick or bite isn't found, your provider will usually take a blood draw or skin and examine the tick (if able).
Your dog can also show signs of having RMSF, like difficulty walking, laziness, poor appetite, and skin discoloration. These symptoms can alert you of a possible infection within you. If your dog shows these symptoms, contact your local veterinarian right away.
How is Rocky Mountain Spotted Fever treated?
If you find a tick latched onto your skin, use tweezers to grab the tick very gently near its head or mouth. Carefully dislodge the tick and preserve it in case your medical provider wants to determine whether it carries RMSF bacteria. If it's still alive, place it into a plastic bag or jar and seal it tightly to bring to the doctor's office for identification. Finally, clean the bitten area and tweezers very thoroughly with antiseptic and wash your hands with hot water and soap.
Rocky Mountain Spotted Fever treatment begins with the antibiotic doxycycline (chloramphenicol, if you're pregnant) immediately—even before your test results come back. This is because rapid, early treatment is necessary before RMSF worsens and creates complications. Common side effects of these antibiotics include diarrhea, nausea, loss of appetite, and a rash.
You're much more likely to avoid further complications if you get treatment within five days of showing symptoms. If your symptoms are or become severe, you'll likely be admitted to the hospital for extra care, as half of all deaths occur within the first eight days.1 You'll be given more tests and IV fluids while your symptoms are monitored.
After antibiotic treatment herbal remedies can be used to relieve nausea (ginger, peppermint, vitamin B6, lemon, and acupuncture. To soothe muscle aches try: magnesium, potassium, calcium, and MSM.
In some cases of RMSF antibiotics fail and the patients continue to suffer. To a conventional doctor the diagnosis and treatment is fairly straightforward, but integrative care practitioners like homeopaths treat the unique characteristics of a patient's condition (taking into consideration other health conditions that may be preventing healing). That's why integrative treatments vary from patient to patient. Some homeopathic treatments for RSF include doxycyclinum, acetaminophen, sepia, and bryonia alba.
You can protect yourself from RMSF by:
- limiting your time in densely wooded areas during tick season
- keeping your lawn well-trimmed and tended
- tucking your pants into your socks and your shirt into your pants
- wearing boots or hiking shoes
- wearing lightly colored clothing so ticks are easier to spot
- using insect repellent containing at least 30% DEET around your armpits, ears, and groin
- performing a careful body check at the end of the day
- carefully inspecting your dog for ticks
- spraying your dog with insect repellent from a pet store
Reserve Your Appointment Now
While Rocky Mountain Spotted Fever is uncommon, people who frequently enjoy outdoor activities or travel to areas with a high infection rate are at a higher risk. If you or someone you know is showing symptoms of RMSF, get medical attention immediately to prevent life-threatening complications.
To speak with a Rocky Mountain Spotted Fever specialist today in Glendale, call (424) 365-1800 or contact Vitality Integrative Medicine online.
Sources:
1. Drexler, Yaglom, Casal, et al. "Fatal Rocky Mountain Spotted Fever along the United States–Mexico Border, 2013–2016 - Volume 23, Number 10-October 2017 - Emerging Infectious Disease Journal - CDC." Centers for Disease Control and Prevention, Emerging Infectious Diseases, 18 Sept. 2017, wwwnc.cdc.gov/eid/article/23/10/17-0309_article.
Vitality Integrative Medicine
Address
4849 Van Nuys BlvdSuite 104
Sherman Oaks, CA 91403
(424) 365-1800
www.vitalityintegrative.com
Hours
Mon:
8:00 am - 6:00 pm
Tue:
8:00 am - 6:00 pm
Wed:
8:00 am - 6:00 pm
Thu:
8:00 am - 6:00 pm
Fri:
8:00 am - 6:00 pm
Sat:
8:00 am - 12:00 pm
